|
|
Case Report
| ||||||
| Epilepsy with hallucinatory phenomena in pediatric age: A case report | ||||||
| Marlene Rodrigues1, Sofia Martins2, Ana Antunes2, Teresa Pontes2, Henedina Antunes3, Ricardo Maré4 | ||||||
|
1Pediatric Resident, Pediatrics Department, Hospital de Braga, Braga, Portugal.
2Pediatric Consultant, Pediatrics Department, Hospital de Braga, Braga, Portugal. 3Pediatric Gastroenterology Senior Consultant and Professor of Pediatrics, Pediatrics Gastroenterology, Hepatology and Nutrition Unit, Hospital de Braga and Life and Health Sciences Research Institute (ICVS), Health Sciences School of University of Minho, Associated Laboratory ICVS/3B's, Braga/Guimarães, Portugal. 4Neurology Consultant, Neurology Department, Hospital de Braga, Portugal. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article: |
| Rodrigues M, Martins S, Antunes A, Pontes T, Antunes H, Maré R. Epilepsy with hallucinatory phenomena in pediatric age: A case report. Case Rep Int 2016;5:44–47. |
|
Abstract
|
|
Introduction:
Hallucinations in children may be part of normal development and not necessarily a symptom of mental illness, but they are subject of great concern to parents and clinicians. They may be a manifestation of a wide spectrum of disorders, such as intoxication, acute febrile illness, endocrinological, neurological or psychiatric disorder.
Case Report: Clinical report of a previously healthy nine-year-old boy presented with visual and auditory hallucinations over the last month. During hospitalization it was performed electroencephalogram, audio record of hallucinatory description and child's illustration of the goblins seen in hallucinations. The etiological investigation excludes other causes, and changes in the electroencephalogram confirmed the diagnosis of epilepsy. The child presented with clinical improvement after treatment with sodium valproate, without recurrence of symptoms. Conclusion: This clinical report intended to emphasize the importance of considering epilepsy as a differential diagnosis in children and adolescents with psychic phenomenology, to make a timely diagnosis and treatment. | |
|
Keywords:
Children, Epilepsy, Hallucinations, Pediatrics
| |
|
Introduction
| ||||||
|
In adults, hallucinations are usually linked to serious psychopathology but in children they are less frequents and not necessarily a symptom of mental disease [1]. A hallucination is a sensory perception in the absence of an adequate external stimulus. They can be elementary as hearing a sound or see a point of light, usually originating in the occipital lobe, or complex, like listening sounds, someone speaking or watching structured pictures/scenes that can occur on seizures originated in occipital, temporal (mesial or mesocortical) or parietal lobes and limbic area [2] [3]. In some cases, the origin of hallucinations is not cortical and may arise from brainstem and amygdala dysfunction. They must be distinguished from similar phenomena such as illusions (altered perception of a real external stimulus), elaborated fantasies and imaginary people [2] [4][5]. Hallucinations in childhood may be triggered in the course of some acute diseases, sometimes also associated with altered state of consciousness, such as febrile illness and intoxications. They can also be a manifestation of neurological diseases, such as migraine or epilepsy, and psychiatric as schizophrenia, depression and anxiety [6] [7] [8]. Hallucinations caused by convulsive disorders are rare and can be somatosensory, visual, auditory, olfactory or gustatory. The diagnosis involves a detailed clinical history and physical examination. Electroencephalogram (EEG) is mandatory, as well as brain magnetic resonance imaging. Hallucinations approach involves the treatment of underlying primary disease [1] [7] [8] [9].
| ||||||
|
Case Report
| ||||||
|
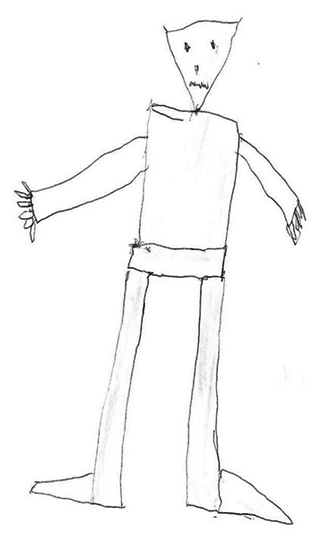
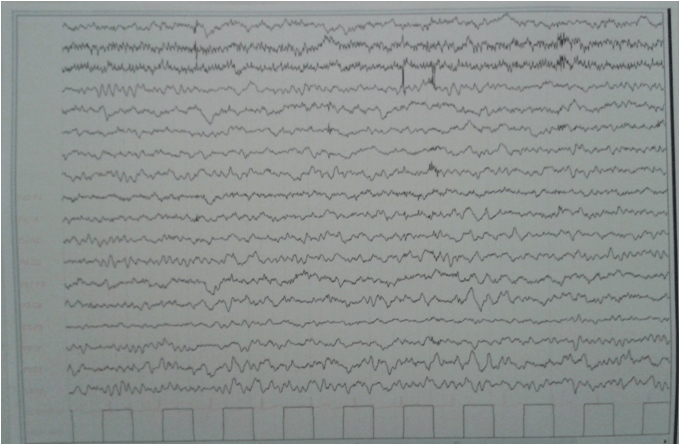
We report a previously healthy nine-year-old boy, with a family history of epilepsy in a paternal aunt, admitted to emergency service of residence area with persistent daily auditory hallucinations, sometimes also visual, occurring in bursts over the last month. He referred that had seen colored monsters and goblins that attacked, screamed and told him to go away; Sometimes he tried to hide himself under the bedclothes so he could not see them and other times he was found closed in the bathroom crying. It was not identified any factor that make seizures worse or better and no postictal symptoms were described. The patient had one isolated determination of fever and diarrhea with no other associated symptoms, at admission day. Analytical study including blood count, ionic and acid-base balance, renal function, transaminases, C-reactive protein and blood cultures did not reveal alterations, as well as urinalysis with negative urine culture. The patient was transferred to our hospital institution for neurology evaluation. On admission, he was thermodynamically stable with normal physical and neurological examination. Lumbar puncture was performed (cells 2, erythrocytes 0, proteins 0.18 g/L) with negative virological (enterovirus, herpes I and II, varicella zoster, cytomegalovirus, Epstein–Barr virus) and microbiological of cerebrospinal fluid. Brain magnetic resonance imaging scan was normal. During hospitalization, after informed consent of legal representative, audio record of hallucinatory description and child's illustration of the goblins seen in hallucinations were made (Figure 1). Video-EEG revealed left and right side epileptiform activity on temporal-parietal-occipital areas (not synchronous). The child was cooperative during the examination. No specific changes were evidenced by hyperpnea and intermittent light stimulation. Neither epileptic seizures nor behavioral changes were observed. The diagnosis of simple partial epilepsy with psychic symptoms (complex visual and/or hearing hallucinations and intense feeling of fear) was established. He had favorable outcome with complete remission of hallucinatory episodes after sodium valproate therapy with dosage of 15 mg/kg per day. The child is being followed-up on consultation and maintains therapy with sodium valproate 20 mg/kg per day. No further episodes of hallucinations were registered. The EEG in the last follow-up, nine months after the diagnosis, showed scarce epileptiform activity on the right centro-parietal area (Figure 2). | ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
Hallucinations in children are subject of great concern and anxiety to parents and clinicians. In adults, they are often synonymous of psychotic illness, but in children can be part of normal development or an acute disease manifestation [1]. In epileptic patients, neuronal discharges at occipital, temporal or parietal lobes and limbic area may result in ictal psychotic phenomena. Psychic phenomenology of epileptic nature must be considered in differential diagnosis of a number of other entities. In a study of 62 children with nonpsychotic source hallucinations, 34% had depression, 22% hyperactivity disorder and attention deficit, 21% behavioral disturbances and 23% other diagnosis [1]. The case we report is an example in which hallucinations are the expression of an underlying disease, in this case epilepsy. Auditory hallucinations indicate, most likely, temporal dysfunction while the complex visual hallucinations, evoking visual memories, are associated with activation of parietal-temporal visual association cortex [9] [10][11]. The fear associated with these phenomena can be related to the hallucination content and/or activation of limbic areas. Seizures associated with hallucinations and fear are often difficult to distinguish from psychiatric disorders, and psychological symptoms are sometimes the "top of the iceberg symptoms," pointing to some less obvious cause. They can mimic a number of other pathologies, delaying the correct diagnosis. Therefore a proper investigation of such symptoms is mandatory. In our case, video-EEG was performed and proved to be essential to confirm the diagnosis, detecting ictal activity, although without observed seizures or behavior disturbs during the examination test. However, it is important to note that EEG is not always able to detect ictal activity in this case, so the video documentation of hallucinations can help to uncover important signs for the differential diagnosis [8]. | ||||||
|
Conclusion
| ||||||
|
Hallucinations in children and adolescents requires a rigorous clinical examination, diagnostic tests and detailed psychological evaluation, to rule out medical causes and identify the psychopathological, psychosocial and cultural factors that may be associated. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Marlene Rodrigues – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version published Sofia Martins – Analysis and interpretation of data, Acquisition of data, Revising it critically for important intellectual content, Final approval of the version to be published Ana Antunes – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Teresa Pontes – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Henedina Antunes – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Ricardo Maré – Substantial contributions to conception and design, Analysis and interpretation of data, Acquisition of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Marlene Rodrigues et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|